
CASE STUDY
Behavioral Health Urgent Care Clinic: Providing Critical Care When and How It’s Needed
An Innovative Model Connecting People with Acute Mental Health and Substance Use Needs to Care

Authors: Laura Knapp, LICSW, Providence Regional Medical Center and Thomas Alfieri, PhD, Purdue Pharma L.P.
The authors thank Mary Drew, founder and CEO of Reality Check, a non-profit in Jaffrey, New Hampshire, and Frederica M. Williams, president and CEO of Whittier Street Health Center in Boston for their insightful comments and suggestions. In addition, the authors acknowledge editorial support from A.M. Samuels, MPH and Padilla, a communications firm specializing in public relations, advertising and multi-media engagement.
Financial Disclosures:
Providence General Foundation, on behalf of Providence Regional Medical Center Everett, applied for and received a grant from Purdue Pharma L.P. (“Purdue”) to implement a two-pronged approach to addressing the opioid crisis in Snohomish County. The portion for establishing and running the Clinic – a two-year pilot effort – is the focus of this case study. All work featured in this case study reflects ongoing efforts to support the development and operation of the Clinic.
Purdue also provided funding to support the development of this case study.
Thomas Alfieri, PhD, is an employee of Purdue.
Executive Summary
After reviewing this case study, readers will have an understanding of how Providence Regional Medical Center in Everett, Washington, developed and launched the Behavioral Health Urgent Care clinic (the Clinic) to provide tailored assessment, immediate treatment and coordination of care for patients experiencing a mental health crisis, including issues related to substance use disorder.
The case study summarizes the model and approach, and reviews the outcomes and lessons learned after its first year of operation.
Below is an overview of the program discussed in this report.
Background
Individuals facing mental health and substance use disorder issues increasingly must turn to emergency departments (ED) to seek care, but these patients require a different set of interventions than acute medical crises and are often challenging to administer in busy EDs. 1, 2, 3
Goals & Approach
- The PRMCE Behavioral Health team sought to address long patient wait times and insufficient care due to lack of mental health providers in Snohomish County by creating an urgent care setting focused on mental health.
- The Clinic, which opened in November 2019, was designed to provide outpatient crisis intervention, initiate treatment and bridge to community mental health providers for ongoing care.
- The patient population were those who needed same-day care but had nowhere to go other than the ED.
Program Elements
- The Clinic is housed on the same campus as the ED, so patients can easily be referred between the two treatment locations based on the type of clinical treatment required. The Clinic team is multi-disciplinary, including a medical director who is a psychiatrist, psychiatric nurse practitioners, a clinical social worker trained in behavioral health, a substance use disorder expert, a peer counselor with lived mental health experience and a receptionist.
- The Clinic provides assessment for each patient, prescribes medication to meet immediate needs, refers to treatment services and ensures coordination of care. If a patient needs medication, the nurse practitioners can prescribe oral medications, including medication-assisted treatment (MAT) for substance use disorder.
Results
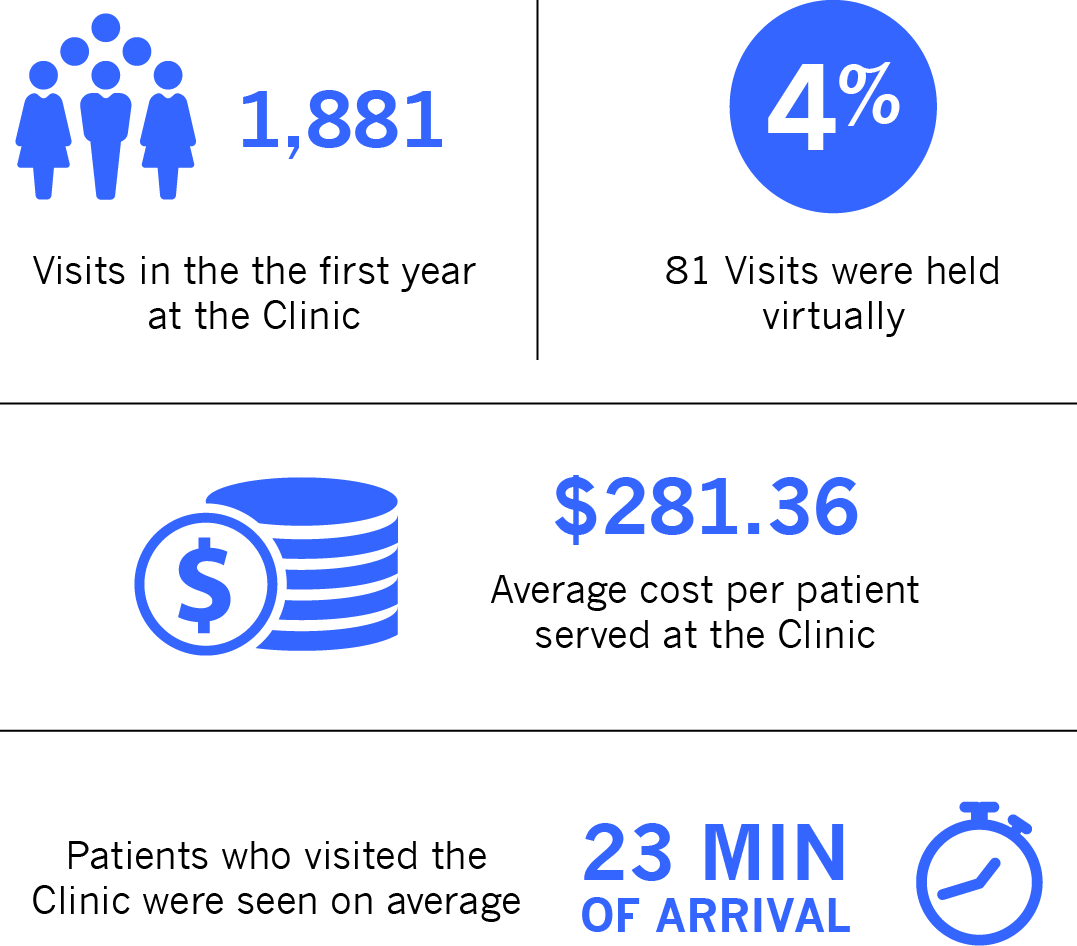
- In its first year of operation (November 2019 to November 2020), the Clinic served 1,688 patients, an average of 6.8 visits per day. Visits lasted 87 minutes on average.
- Nearly 40% of patients reported that they would have gone to the ED for care if the Clinic did not exist.
- Avoidable behavioral health visits to the PRMCE ED decreased by 11% after the opening of the Clinic. A Clinic visit costs less than half of a behavioral health visit in the ED, and patients reported a high level of satisfaction with their care in the Clinic.
- Despite the challenges of service provision during a pandemic, the Clinic has proved to be an effective model for hospitals to provide critical care in a non-ED setting.
The Clinic met its goal of providing critical services for patients with mental health and substance use disorders, reducing avoidable visits to the ED and helping patients get the care they need when they need it.
Behavioral Health Treatment Gaps Are Pervasive in the United States
Building a Bridge to Treatment and Recovery
“No.” It’s a word that patients seeking care for mental health and/or substance use disorder hear all too often while navigating the healthcare system, according to Jordan Larkin-Sinn, a peer counselor at the Behavioral Health Urgent Care clinic (the Clinic) at Providence Regional Medical Center. At the Clinic, Jordan grounds the patient experience in affirmation, right from the start.
“I’m here to listen.”
“I’ve been where you are. You’re not the only one.”
“It’s okay not to be okay.”
Larkin-Sinn has personal experience with the mental health system. He understands that it’s not easy to ask for help, especially in moments of crisis – and what a difference it can make to hear words of comfort and understanding.
“A lot of people who come to the Clinic don’t want to be here. They’re scared. We reassure them that we can be that helping hand.”
Patients seeking urgent care for mental health and/or substance use disorder often have only two choices. If they have an established provider, they can make an appointment – which isn’t always possible on the same day – or go to the emergency department (ED), which can be an overwhelming and stressful environment for patients. The Clinic seeks to offer patients a third option for urgent care delivered in a supportive environment.
“Patients have told me about traumatic experiences sitting in the ED for more than 36 hours waiting to talk to a crisis counselor. It’s horrible to sit there for so long and not get the help you need. Our goal is to keep them out of the ED and bridge them to other support and guidance.”
The Clinic offers a supportive environment where, even when patients aren’t sure what they need, they can find a trusted guide. In addition to addressing immediate care needs, the staff helps patients and families learn the language, chart a path forward and work around roadblocks.
“There are so many ‘no’s’ out there. Patients get to a point where they just stop asking questions – and they might turn to other things that just create more problems. It’s such a big change when people come into our clinic. We are here to help, we understand, and we’re ready to get them on the path of feeling better. You can watch the weight on their shoulders be lifted away.”
The Clinic equips patients and families with the resources they need to overcome barriers to care and take their next steps on the journey to treatment and recovery.
National Behavior Health Challenges
There is a growing, nationwide need for behavioral health services delivered in an urgent care setting that address mental illness and substance use.
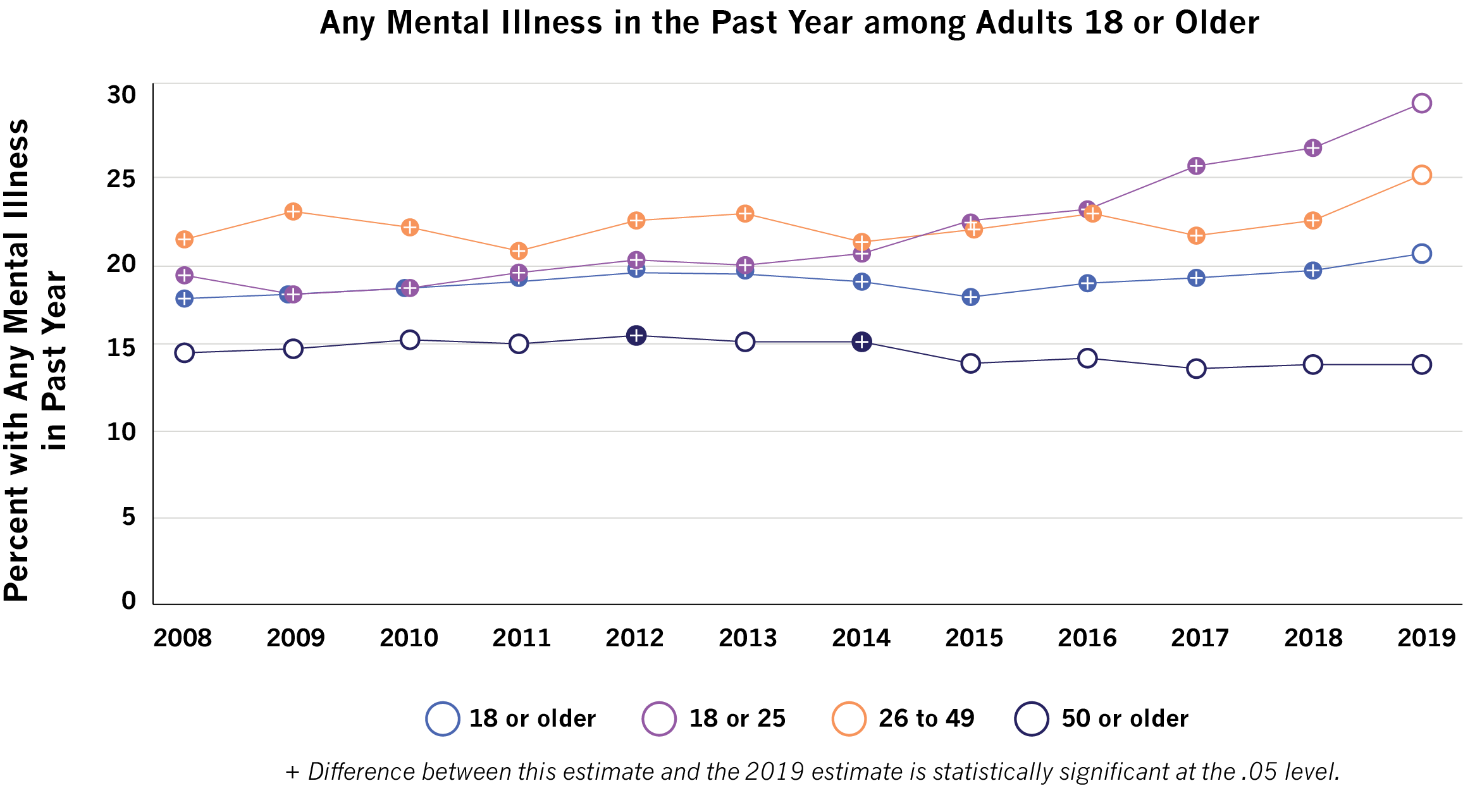
The prevalence of mental illness and substance use disorder among adults has been increasing in the United States, even prior to the COVID-19 pandemic. The 2019 National Survey on Drug Use and Health (NSDUH) published by the Substance Abuse and Mental Health Services Administration (SAMHSA) reports that 25% of U.S. adults (61.2 million people) had either a mental illness or substance use disorder in the past year.4 This includes a significant increase in adults with mental illness over the past decade – from 39.8 million (17.7%) in 2008 to 51.5 million (20.6%) in 2019 (figure on the bottom).4
And online screening data from Mental Health America – a national community-based nonprofit that promotes mental health – shows significantly higher numbers and more serious indicators of mental illness from January to September 2020 when compared to the same period in 2019.5
According to the National Institute on Drug Abuse, about half of those who experience a mental illness will experience substance use disorder at some point in their lives and vice versa.6
The relationship between substance use disorders and mental disorders is bi-directional – the presence of one may contribute to the development or exacerbation of the other.4 People who have both disorders together tend to have worse impairment than people with either disorder alone, and they have worse treatment outcomes.4 The 2019 NSDUH found a significant increase in the number of adults aged 18 years or older with both mental illness and substance use disorder between 2015 and 2019, from 8.1 million to 9.5 million.4
There are significant gaps in meeting mental health and substance use care needs.
The 2019 NSDUH shows that about a quarter (26%) of the 51.5 million adults who have a mental illness report they have at least some level of unmet need for mental health services, and 5.8 million have not received any services at all.4 Among the 13.1 million adults who report a serious mental illness in the past year, almost half (48%) did not get needed healthcare services.4 The same government survey shows that 21.6 million people aged 12 years or older needed substance use treatment, but only 4.2 million received it.4
Adults without mental illness also face considerable barriers. Over half (56%) of adults have sought or wanted to seek mental health treatment for themselves or others. They face a number of obstacles, but getting an appointment is the biggest hurdle. More than one-third (38%) have had to wait longer than one week for access to mental health services, and nearly half (46%) have had to or know someone who has had to travel more than one hour roundtrip to access services.
While demand for mental health and substance use care is increasing, there is a nationwide shortage of psychiatrists.7 In 2018, the federal government estimated that the U.S. needed nearly 7,000 additional psychiatrists to provide treatment to those who need it across the country.7

Individuals facing mental health issues and substance use disorders increasingly have to turn to emergency departments (EDs) to seek care.
Insufficient funding for community-based and outpatient programs combined with insurance barriers forces patients to seek care in emergency settings.1 The problem is not small: about one in eight ED visits involves mental health or a substance use disorder and the proportion appears to be increasing.2
EDs are not designed to meet the needs of these patients, and that often leaves them waiting hours or even days for appropriate care.1,8 Although treating physical and behavioral health issues together can improve patient experience and outcomes,9 mental health and substance use issues require a different set of interventions than acute medical crises and are often challenging to administer in a busy ED.3 The Behavioral Health Urgent Care clinic (the Clinic) at Providence Regional Medical Center in Everett, Washington (PRMCE), the subject of this case study, was designed to provide an innovative model of care to connect those in need to appropriate services in a timely and effective manner. The Clinic has proven to be especially valuable to patients in the midst of a prolonged pandemic, which is increasing stress and isolation.10
Behavioral Health Needs in Washington State and the Everett Area
Located north of Seattle, Snohomish County, the area that PRMCE serves, has a ratio of 310 patients to one mental health provider, which includes psychologists, licensed clinical social workers, psychiatrists, counselors, marriage and family therapists, mental health providers who treat alcohol and drug abuse, and advanced practice nurses specializing in mental health care.11 This ratio is lower than Washington state’s average of 270 patients per provider.11 In a January 2019 report, the Snohomish County Health District estimated that between 5,000 and 10,000 of its residents had opioid use disorder and up to 80,000 were misusing opioids.12
The problem was evident to healthcare administrator Laura Knapp, a licensed clinical social worker who helped spearhead the new Behavioral Health Urgent Care and is PRMCE’s director of behavioral health. “The gap between mental health and substance use needs and available care led to some patients, even those who were already established in an outpatient practice, sometimes having to wait months to see their healthcare provider.” Another barrier is that many practices are limited in insurance they accept – which can exclude Medicaid patients. This leaves many patients who need medical or therapeutic intervention to stabilize a psychiatric crisis with nowhere to turn other than the Providence Regional Medical Center ED.

Fast Facts
Providence Regional Medical Center Everett
Established in 1905
Everett, Washington
501c3 non-profit
AFFILIATIONS
PRMCE is part of Providence Health & Services-WA, the largest healthcare provider in Washington state with a comprehensive network of facilities and services across the lifespan.
- More than 75% of the PRMCE patient population resides in Snohomish County, which is largely rural. PRMCE also serves residents of surrounding counties including Skagit, Whatcom, Island and San Juan.
- Snohomish County residents are predominantly white (73%), 12% Asian, 11% Hispanic, 5% mixed race, 5% other, 4% Black, 1% American Indian and 1% Pacific Islander.
- PRMCE is a full-service acute care tertiary hospital with 595 beds.
- The ED at PRMCE is larger than a football field, averaging 60,000 visits per year, and is the second busiest in the state.
Providence Regional Medical Center Everett
PRMCE, part of Providence Health & Services-WA, the state’s largest healthcare provider, is a full-service medical center offering cardiology, neurology, cancer treatment, a birthing center and a Level 2 Trauma Center serving patients from several counties in northern Washington. As of July 2021, it also has a 24-bed inpatient psychiatric department that complies with state requirements for psychiatric care. PRMCE is located in Everett, the largest city in Snohomish County and home to approximately 113,000 residents.
Even prior to having an inpatient behavioral health unit, PRMCE has cared for a large number of mental health patients, including individuals with co-occurring medical, mental or substance use needs. In 2019, 15,386 patients with a behavioral health diagnosis (including 3,901 with opioid or other substance use disorder diagnosis) came into or through the ED, which averages approximately 60,000 visits per year. Patients visiting the ED for behavioral health are seen for a variety of clinical presentations which may include treatment for substance use disorders, anxiety, depression or psychosis – challenges which are exacerbated by the environment of a busy Level 2 Trauma Center.
The Behavioral Health Urgent Care Program
Identifying the Service Gap
In 2019, a Community Health Needs Assessment was conducted by PRMCE with the goal of identifying unmet health and mental health challenges among community members. It found a 27% increase in poor mental health days (days where patients report feeling stress, depression, and problems with emotions) per month since 2017, with an average of 4.1 debilitating days per month that Snohomish County residents were unable to do their usual activities due to poor physical or mental health.13 It also found that the top diagnosis for avoidable outpatient emergency room visits is for alcohol and drug abuse13. The assessment concluded that patients experience long wait times or insufficient care due to lack of mental health providers13, and identified access to mental health care and opioid use disorder as the top two significant health-related needs for their patient population13. These conclusions were further confirmed by PRMCE Behavioral Health team’s partners providing community mental health and substance use disorder services.
Therefore, the team envisioned an urgent care type setting to close this critical gap and set out to develop their model and secure funding for its startup. PRMCE applied for and received a grant from Purdue to implement a two-pronged approach to addressing the opioid crisis in Snohomish County. The portion for establishing and running the Clinic – a two-year pilot effort – is the focus of this case study. All work featured in this case study reflects ongoing efforts to support the development and operation of the Clinic.
“It was clear to us that there were not enough access points in our systems for people with behavioral health needs. Our Clinic not only fills this void, but we provide an innovative approach to care once they’re here.”
— Danielle Waldron, ARNP, RN, psychiatric nurse practitioner, Behavioral Health Urgent Care
Goals & Approach
The PRMCE team conceptualized an outpatient urgent care clinic that would provide crisis intervention, initiate treatment, and bridge to community mental health providers for ongoing care. The intention was to serve those who needed same-day care but had nowhere to go besides the ED. Although the team knew there would be some who required ED services, the goal was to reduce the burden on the ED while providing an alternative treatment setting more conducive to mental health crisis intervention.
The Clinic was modeled after the Pediatric Behavioral Health Urgent Care Center at Cohen Children’s Medical Center in New York City, which provides access, engagement, specialty assessment, coordination, and transitional care. PRMCE learned of the Cohen Children’s model through its involvement in the Institute for Health Improvements ED and UP Collaborative to address behavioral health challenges in EDs. At the time the Clinic was conceived, there were very few known behavioral health urgent care clinics in U.S. hospital settings for adults. Knowing that another provider had plans to open a pediatric behavioral health clinic nearby, PRMCE focused on the adult patient population.
Program Elements

Location & Hours
The Clinic is housed on the same campus as the ED, so patients can easily be referred between the two treatment locations based on the type of clinical treatment required.
There are four exam rooms and a large waiting room to allow spacing for patients in crisis. For the first year of operation (November 2019 to November 2020), clinic hours were Monday through Friday, from 10:00 a.m. to 5:00 p.m. The start time was chosen due to low volume in the ED during early mornings and the need for coverage in late afternoons. No appointments are necessary, and patients are seen on a first come, first served basis.
As a result of the COVID-19 pandemic, beginning in April 2020 virtual visits were also offered.
Staffing
The staffing structure was designed to include clinicians with expertise in both mental health and substance use disorders to serve an anticipated 1,000 clinic visits in the first year, or approximately four visits each day. The Clinic team is multi-disciplinary, including a medical director who is a psychiatrist, one full-time and two part-time psychiatric nurse practitioners, a clinical social worker trained in behavioral health, a substance use disorder expert, a peer counselor with lived mental health experience, and a receptionist. New staff were hired upon opening, along with current PRMCE leadership (both the medical director and director of behavioral health were currently employed by PRMCE when the Clinic opened). In addition to their clinical training, all staff are trained in trauma informed care. The team works collaboratively to develop treatment plans tailored to patients’ needs.
Services
The Clinic was designed to provide a tailored assessment for each patient, prescribe medication to meet immediate needs, referral to treatment services, and ensure coordination of care. If a patient needs medication, the nurse practitioners can prescribe oral medications, including medication-assisted treatment (MAT) for substance use disorder. The Clinic works collaboratively with multiple programs that treat SUD for ongoing treatment, including facilitating access to residential treatment and referring to an ongoing MAT prescriber.
Costs & Fees
The Clinic was established as an outpatient clinic to allow for credentialing with individual payers. PRMCE provides quality care to all regardless of ability to pay. Patients who do not have insurance are referred to the Patient Financial Assistance Program that provides free or discounted services to eligible patients.
Stakeholder Engagement
PRMCE’s Executive Leadership Team and Providence General Foundation were supportive of the creation of the Clinic. PRMCE provided space for the Clinic and the Foundation applied for funding from Purdue as well as paid for the furniture. The team also worked with community providers of mental health services to raise awareness about the Clinic and coordinate care for patients following crisis intervention in the Clinic. These partners come from diverse settings, including treatment and recovery services, behavioral health nonprofits, community mental health programs, psychiatric facilities, health districts, county health and primary care.
Year 1 Implementation
Operations
“The Clinic is a net for those who might slip through the cracks. They fall through to us. Sometimes just getting some education and normalizing their reactions helps, telling them here are some tools to manage, here are some resources, let’s talk about medication.”
— Crystal Blankinship, LICSW, manager of behavioral health, Providence Medical Group
The Clinic opened its doors to the public on November 4, 2019. The first case of COVID-19 in the U.S. was reported in Snohomish County just over two months later, on January 20, 2020.14 Despite the challenges the Clinic faced during the pandemic, it remained open throughout its first year. By the end of November 2020, the Clinic had served 1,688 patients – well over what was anticipated.
Most patients were seen in person. Because many community health agencies in the area were not able to offer in-person treatment once the COVID-19 pandemic began, the Clinic became a critical source of services for patients who might have challenges seeking appropriate care virtually. Patients could walk in without an appointment Monday through Friday, from 10:00 a.m. to 5:00 p.m. and were usually seen the same day. Beginning in April 2020, they could also call to make an appointment for a same-day virtual visit. Although virtual visits were encouraged by Clinic staff, very few patients chose this option. Of the 1,881 visits completed in the first year, only 81 (4%) were virtual. In rare cases, visits were conducted by phone for established patients who required follow-up but were not able to connect virtually. According to Providence, the average cost per patient served at the Clinic was $281.36, less than half of the cost of a behavioral health visit in the ED.
Patients visiting the Clinic were seen within 23 minutes of arrival, on average. Once the pandemic began, patients were asked to wait in their cars until a private room was available. All safety protocols were followed (cleaning, PPE, distancing, masks) to ensure patient and provider safety. When Clinic staff were unable to work due to pandemic-related factors, hospital staff provided floating coverage on a per diem basis.
Upon patient arrival, the peer counselor met with patients to understand the reason for seeking care. This information was shared (in person) with the multi-disciplinary team who then decided collaboratively who would see the patient first based on the patient’s needs. Patients may receive counseling and support for acute symptoms, a prescription for psychiatric medications when indicated, and assistance accessing social services such as referrals to ongoing behavioral health services, substance use disorder recovery services, basic needs, and domestic violence support services. Staff located a community mental health provider that would meet the longer-term needs of the patient and supported patients in scheduling appointments to ensure a smooth handoff with that next organization. Once a patient was connected, the peer counselor contacted patients after their visits to inquire if they were encountering barriers to care.
Service Utilization
As intended, patients came to the Clinic directly rather than going to the ED. Awareness about the Clinic was raised through PRMCE internal and external newsletters, local media, social media, and outreach to and through community partners such as Providence Medical Group neighborhood clinics throughout Snohomish County, Compass Health, Swedish Medical Center Edmonds ED, Community Health Center of Snohomish County and Sea Mar Community Health Centers. Many patients were referred from the Volunteers of America Western Washington crisis line (emotional support crisis services available 24/7), community behavioral health service providers, social service agencies, diversion centers, primary care providers and health clinics. One-third of patients lived in Everett, the largest city in Snohomish County.
Only about 7% of patients were referred directly by the ED for same-day visits. All patients who seek treatment at the ED are seen by a physician for evaluation. Patients who are not admitted may be walked to the Clinic for coordination of care. When patients have medical issues or are in very acute crisis and out of safety – for themselves or others – they remain in the ED. In addition, the Clinic is also receiving patients from the Swedish Edmonds ED (approximately 18 miles away) for follow-up visits.
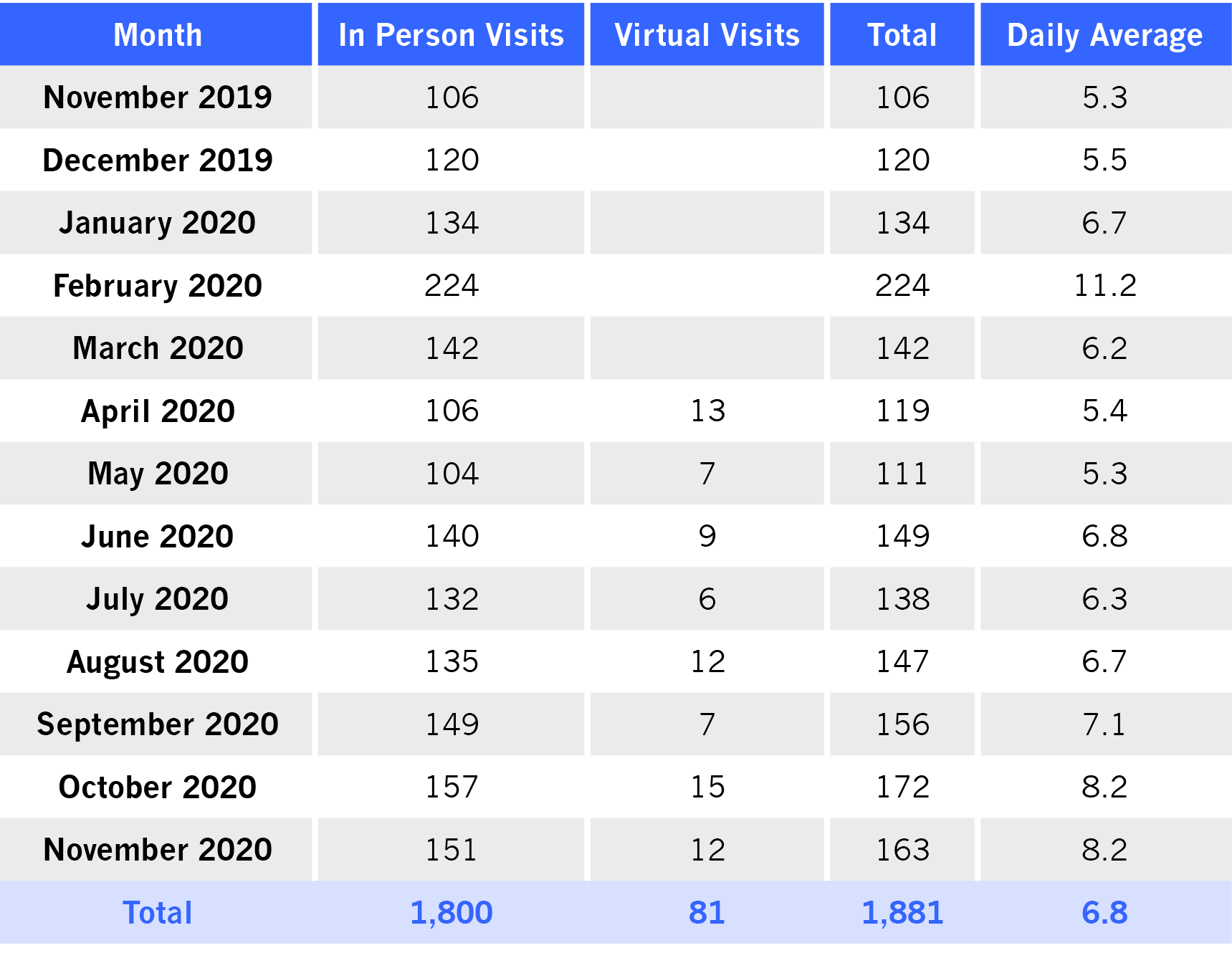
The Clinic averaged 144 visits per month and 6.8 visits per day across the first year. The majority of patients required only one visit and connection to community service providers; but in some cases, patients needed additional support while waiting for access to providers who were backlogged.
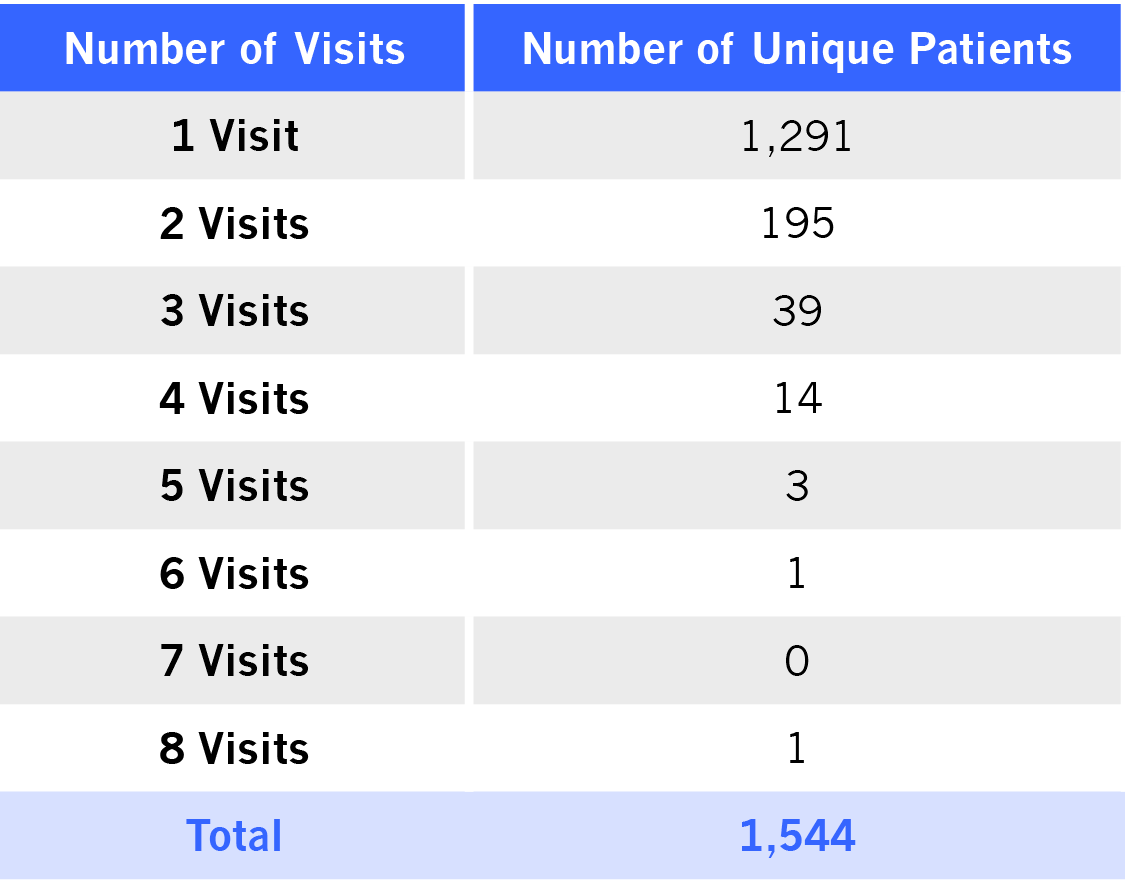
During the first year of operations, the Clinic served 1,688 unique patients (in-person and phone visits). Without phone visits (but including virtual office visits), the Clinic served 1,544 unique patients – including 16% of patients with repeat visits.
Patient Count by Number of Visits November 2019 to November 2020
Unique Patient (in-person and virtual office visits only; excluding phone visits)
As more people became aware of the Clinic, there was a steady increase in service utilization, with an average of 11 visits per day in February 2020. When the pandemic lockdowns began in mid-March 2020, patient volume decreased. However, as the pandemic persisted and there was prolonged stress, anxiety, isolation and barriers to community mental health services, there was a slight upswing in patients who needed crisis services in fall 2020. Unlike many community behavioral health clinics that closed or provided virtual visits only, the Clinic stayed open as well as provided virtual visits. Staff also supported a quarantine site for individuals with COVID-19 diagnoses and housing insecurity in Everett during the pandemic, providing support and MAT to patients as needed.
Duration of Visits
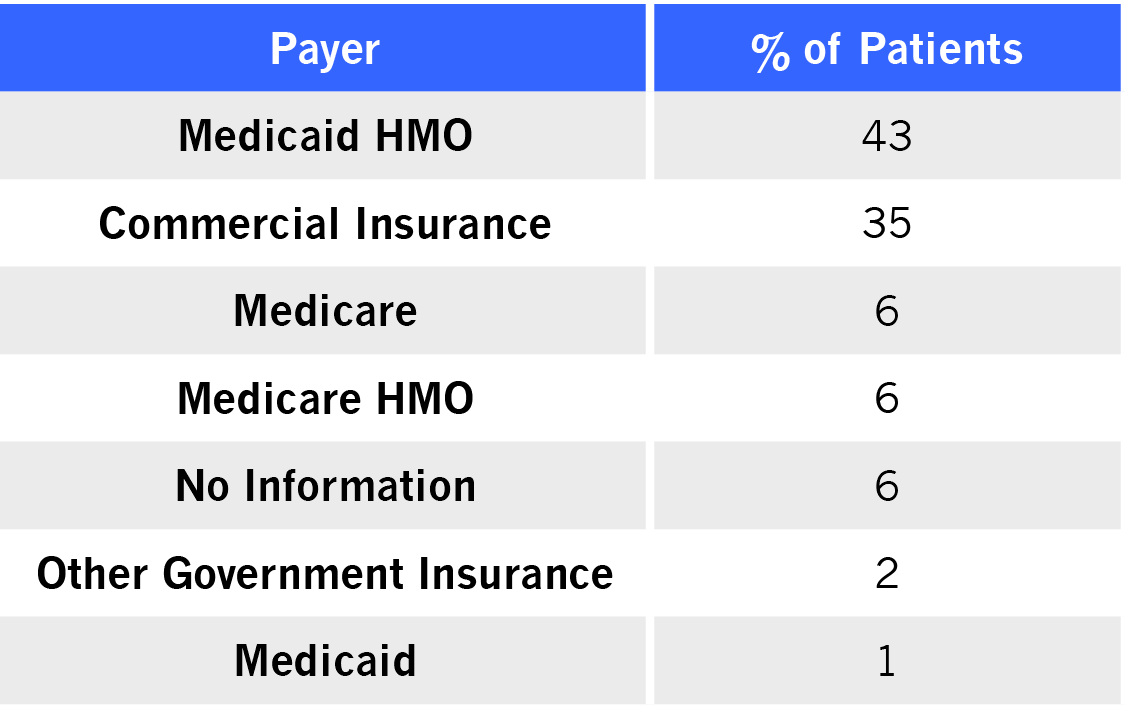
Payer Mix November 2019 to November 2020
Patients spent about 87 minutes on average at the Clinic, with most of this time (64 minutes) in the treatment room and about 36 minutes with a provider. This is approximately a third of the time that a patient might spend in a typical ED visit.
Since a driving philosophy for moving to the Clinic approach is to remove stigma, all patients were served regardless of ability to pay. Almost all (93%) patients had some form of insurance. The high proportion of Medicaid recipients was expected given the documented challenge for these patients in accessing other community mental health services.
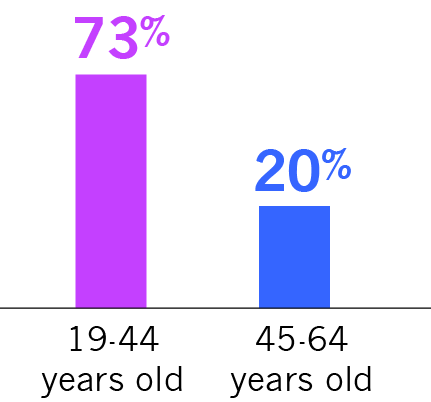
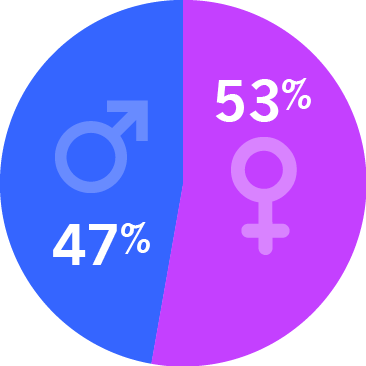
Patient Characteristics
Reasons for visiting the Clinic
Most frequent diagnoses November 2019 to November 2020
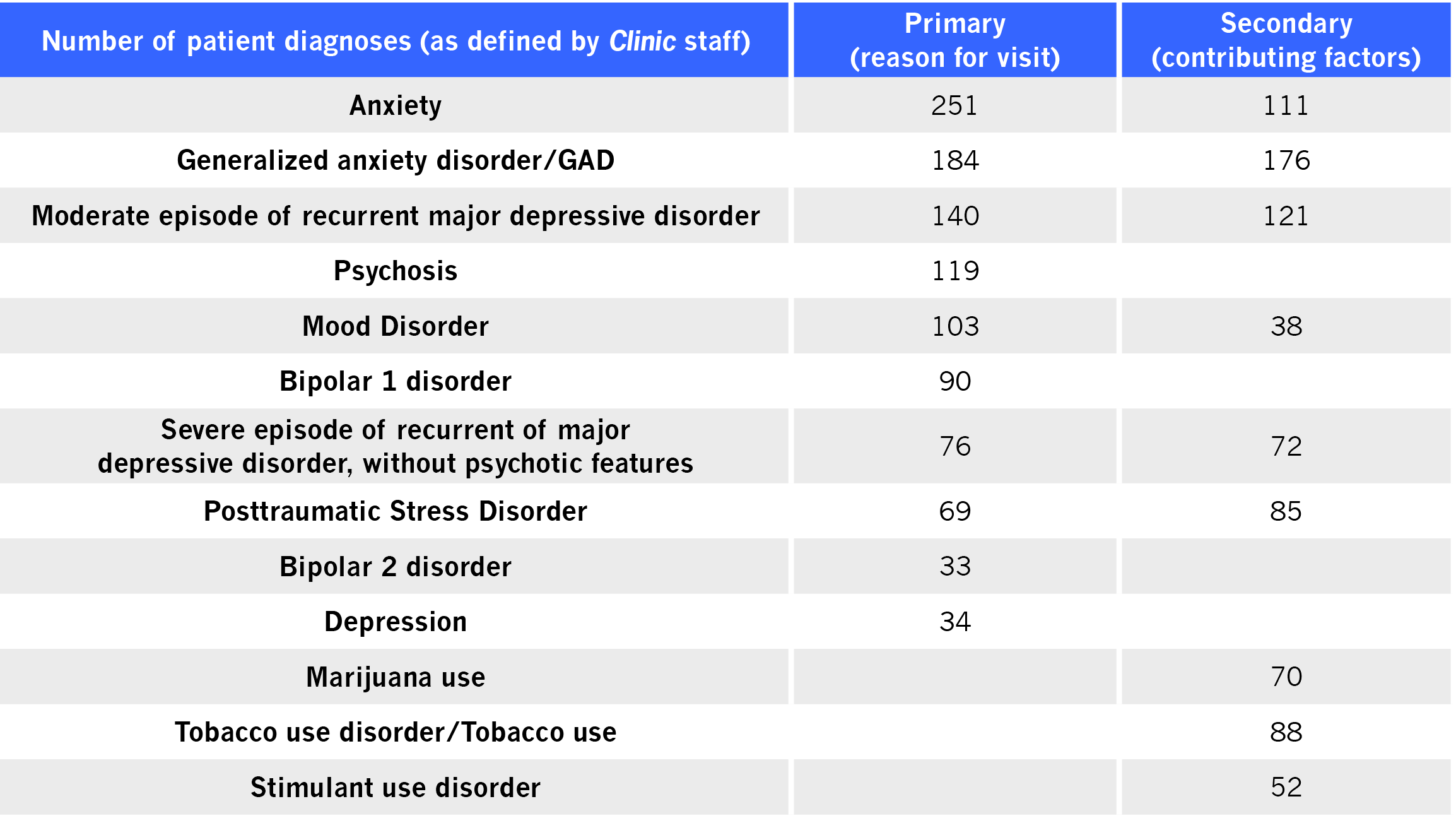
While the Clinic’s patient diagnoses were generally aligned with mental illness prevalence among adults15, the proportion of anxiety and GAD is much higher than what is usually seen – but not surprising given the COVID-19 pandemic.
The top behavioral health diagnoses during the same period in the ED were:
- alcohol-related disorders
- substance-related disorders
- suicide/intentional self-inflicted injury
- schizophrenia
- other psychotic disorders
This suggests that patients with anxiety and mood disorders were more likely to seek care from the Clinic than those in crisis or dealing with alcohol and substance use disorders.
A separate search of electronic health records revealed that among all patients seen at the Clinic, only 67 had an opioid use disorder diagnosis, which was not necessarily a direct contributing factor to the patients’ Clinic visit. The number of patients with a diagnosed opioid use disorder was lower than expected. This may be due to the severely acute state many patients are in when they seek treatment for opioid use disorders (often requiring ED intervention) as well as the Clinic not being open during evenings and weekends (when there is most need for treatment).
Patient Satisfaction
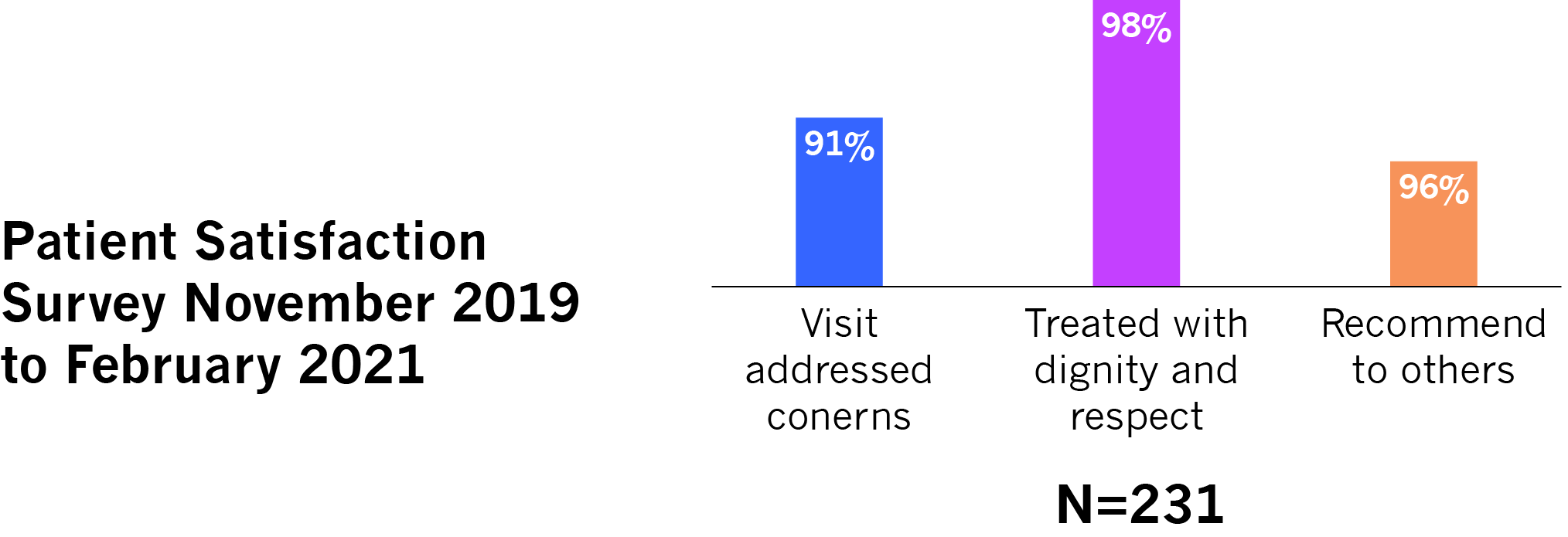
The quiet and calm environment designated specifically for behavioral health made seeking services more socially acceptable and the tailored and trauma- informed approach used by the Clinic made patients feel heard and respected.
“You’ve given me hope for my future. An absolute Godsend.”
“Thank you. I will tell my friends and family because it is difficult to find help right now.”
“Just couldn’t thank them enough for their kindness and resources, suggestions, and allowing me to vent.”
“I felt comfortable enough to express everything I needed to say. ”
“I was able to address everything here at [the Clinic]. In previous visits at other places, I don’t feel people listened like they should.”
Program Outcomes
Nearly 40% of patients surveyed (from November 2019 to February 2021) reported that they would have gone to the ED if the Clinic were not available. The remainder would likely have not gotten any treatment or had to wait, since finding appointments with providers became even more challenging as the pandemic persisted.
“I am an ED nurse who brought my daughter here. She was not in crisis, but we had exhausted any ways to access behavioral/mental health service. This was the best urgent care visit I have ever had for any problem!”
— Mother of Patient
“A lot of the community partners really see us as this space that is able to capture their patients, if they’re falling through the cracks or have fallen off their radar. To get that patient reconnected with their ongoing care.”
— Crystal Blankinship, LICSW, manager of behavioral health, Providence Medical Group
Data from the ED indicate that avoidable behavioral health visits have decreased since the Clinic opened.16 However, acuity increased with the COVID-19 pandemic, based on admit rate data following a mental health diagnosis.
The average number of avoidable visits per month from November 2018 to October 2019 was 350, compared to an average of 310 avoidable visits in the year following opening of the Clinic in November 2019; representing a 11% decrease in avoidable visits.
Avoidable PRMCE Emergency Department Behavioral Health Cases
November 2018 to November 2020
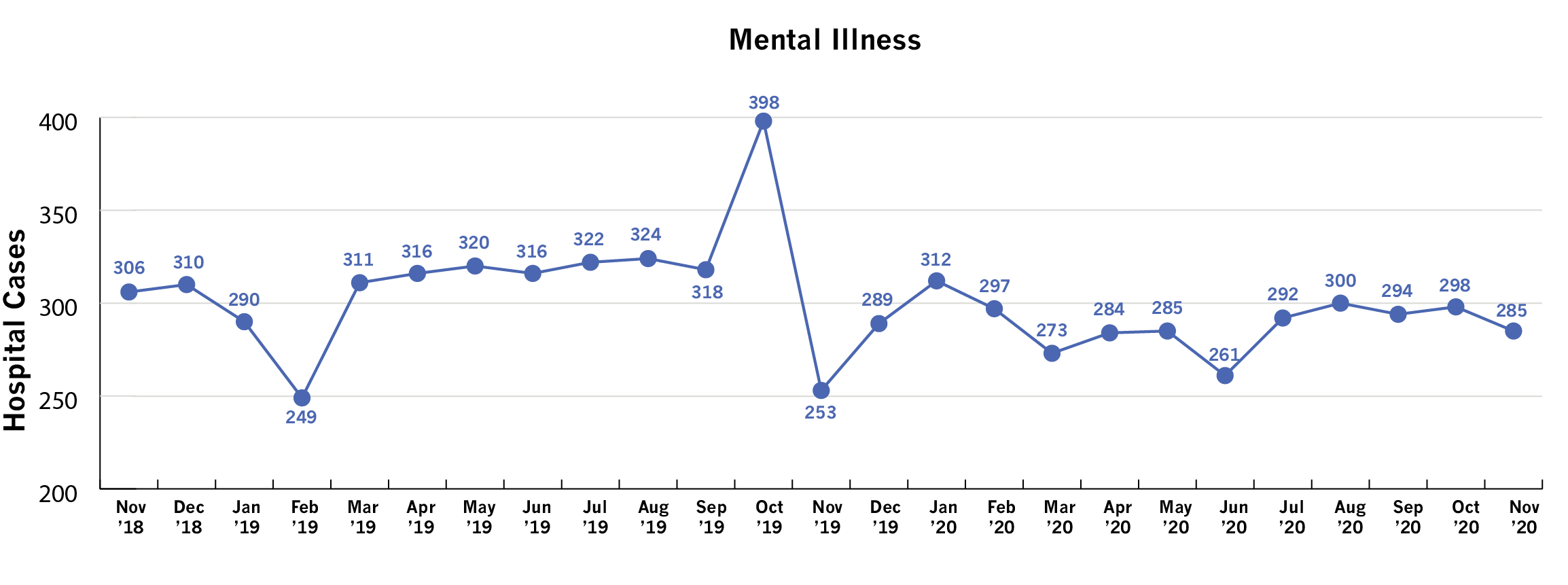
Discussion
The Clinic met its goal of providing critical mental health services for patients in need. In patient surveys, nearly 40% of Clinic patients self-reported that they would have gone to the ED, which is consistent with the magnitude of the observed reduction in avoidable visits to the adjacent ED. The Clinic also helped prevent patients from being untreated or undertreated by an already overwhelmed community mental health system that was further affected by the pandemic.
“We’re here for the community and finding that folks are saying, ‘I was told to come here, wasn’t sure what to do, didn’t want to go to the ED,’ and we are then able to intervene a little sooner.”
— Crystal Blankinship, LICSW, manager of behavioral health, Providence Medical Group
While many community providers closed their doors and shifted to phone and virtual visits, not all individuals had access or felt comfortable with telemedicine – especially when in crisis. The Clinic’s ability to stay open to see patients in person served as an invaluable resource for those community members.
The location of the Clinic near the ED and collaboration between the two were integral to keeping the Clinic open. It not only eased cross-referral based on patient needs but maximized the use of qualified providers and reimbursement of costs across the two treatment settings. Expanding hours of operation during weekends and evenings will help the Clinic continue to provide care when patients experience the most need for services.
Balancing the supply of providers with the demand for same-day services was a challenge. Allowing staff to float between the Clinic and ED helped address this but required staff with medical experience. Certain insurance providers also have stringent requirements on the types of providers that can bill in each treatment setting. This was an important lesson learned, as the substance use disorder professional was unable to bill for services in the Clinic outpatient setting. Maximizing cost reimbursement also addressed another key challenge for the Clinic: high cost and low reimbursement for services. The amount of follow- up and coordination of care to ensure patients are connected to necessary treatment was well beyond what is covered by most insurance.
Establishing bi-directional partnerships with community mental health providers was also integral to the success of this model. Community mental health providers – many of whom were not able to see patients in person – connected patients in acute need to the Clinic, which in turn connected patients to ongoing care from community partners once they had been stabilized. Without these relationships in place, the Clinic would not have been able to serve as the intended bridge across service gaps.
Lastly, the central thread through all these factors is the need for a strong team with different types of skills and experiences to serve patients in crisis, work flexibly across treatment settings, and maintain strong relationships with community partners. Given the high intensity and pace of working with patients in crisis five days per week, it is also critical to support staff wellness. Two ways the Clinic does this is by securing budget to hire per diem support when necessary, ensuring adequate coverage for staff on both short-term and long-term leave, and hiring staff who can transition to other roles as needed. For example, the Clinic manager is also a social worker who can see patients when needed.
“Thank you for taking time to possibly save someone’s life.”
— Patient
Conclusion
Looking Ahead
References
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6754202/
2. Weiss AJ, Barrett ML, Heslin KC, et al. Trends in Emergency Department Visits Involving Mental and Substance Use Disorders, 2006–2013: Statistical Brief #216. Agency for Healthcare Research and Quality. AHEQ. 2016. (p 1) (p1)
https://www.ncbi.nlm.nih.gov/books/NBK409512/
3. Bender D, et.al. A Literature Review: Psychiatric Boarding; Prepared for U.S. DHHS. 2008. (p16) (16)
https://aspe.hhs.gov/system/files/pdf/75751/PsyBdLR.pdf.
4. SAMHSA. Key Substance Use and Mental Health Indicators in the United States: Results from the 2019 National Survey on Drug Use and Health.2020. (p 46) (p44) (p63) (63) (46) (61) (62) (50-51) (See comment on page 12)
https://www.samhsa.gov/data/sites/default/files/reports/rpt29393/2019NSDUHFFRPDFWHTML/2019NSDUHFFR1PDFW090120.pdf
5. 2021 The State of Mental Health in America. Mental Health America. 2020. (p 33) (15)
https://mhanational.org/issues/state-mental-health-america
6. NIDA. Part 1: The Connection Between Substance Use Disorders and Mental Illness. 2020. (p 2)
https://www.drugabuse.gov/publications/research-reports/common-comorbidities-substance-use-disorders/part-1-connection-between-substance-use-disorders-mental-illness
7. Association of American Medical Colleges. The complexities of physician supply and demand: projections from 2018 to 2033. 2020. (p 36) (36)
https://www.aamc.org/system/files/2020-06/stratcomm-aamc-physician-workforce-projections-june-2020.pdf
8. American College of Emergency Physicians. Mental Health. Accessed March 23, 2021.
https://www.emergencyphysicians.org/article/mental-health/mental-health-overview
9. American Hospital Association. Issue Brief: Integrated Behavioral Health is High-value Care. 2019. (p3)
https://www.aha.org/system/files/media/file/2019/12/value-initiative-issue-brief-integrated-behavioral-health-high-value-care.pdf
10. Washington State Department of Health. Statewide high-level analysis of forecasted behavioral health impacts from COVID-19. DOH 820-101. September 2020. (p1) (1) (1,9)
https://www.samhsa.gov/data/sites/default/files/cbhsq-reports/Washington-BH-BarometerVolume5.pdf
11. Washington County Health Rankings Health Rankings. Countyhealthrankings.org. Accessed March 23, 2021. (p2) (1)
https://www.countyhealthrankings.org/app/washington/2020/measure/factors/62/data
12. Snohomish Health District. Opioid use disorder and opioid misuse in Snohomish County. December 2018. (p15)
http://www.snohd.org/DocumentCenter/View/1773/Burden-of-Disease-Report---December-2018-PDF.
13. 2019 Community Health Needs Assessment: Providence Regional Medical Center Everett. PRMCE. (p 16-17) (53) (35) (51)
14. Holshue ML, DeBolt C, Lindquist S, et al. First Case of 2019 Novel Coronavirus in the United States. N Engl J Med. 2020 Mar 5;382(10):929-936. (p2)
https://www.nejm.org/doi/full/10.1056/NEJMoa2001191
15. NAMI. Mental Health by the Numbers. 2019. Accessed Nov 24, 2020. (p 2) (2)
https://www.nami.org/mhstats
16. Hsia RY, Niedzwiecki M. Avoidable emergency department visits: a starting point. Int J Qual Health Care. 2017 Oct 1;29(5):642-645. (p 1)
https://doi.org/10.1093/intqhc/mzx081
17. Centers for Disease Control and Prevention. Coping with Stress. January 22, 2021. https://www.cdc.gov/coronavirus/2019-ncov/daily-life-coping/managing-stress-anxiety.html
18. Kopelovich SL, Monroe-DeVita M, Buck BE, et al. Community Mental Health Care Delivery During the COVID-19 Pandemic: Practical Strategies for Improving Care for People with Serious Mental Illness. Community Ment Health J. 2021 Apr;57(3):405-415. (p1)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7304659/
